
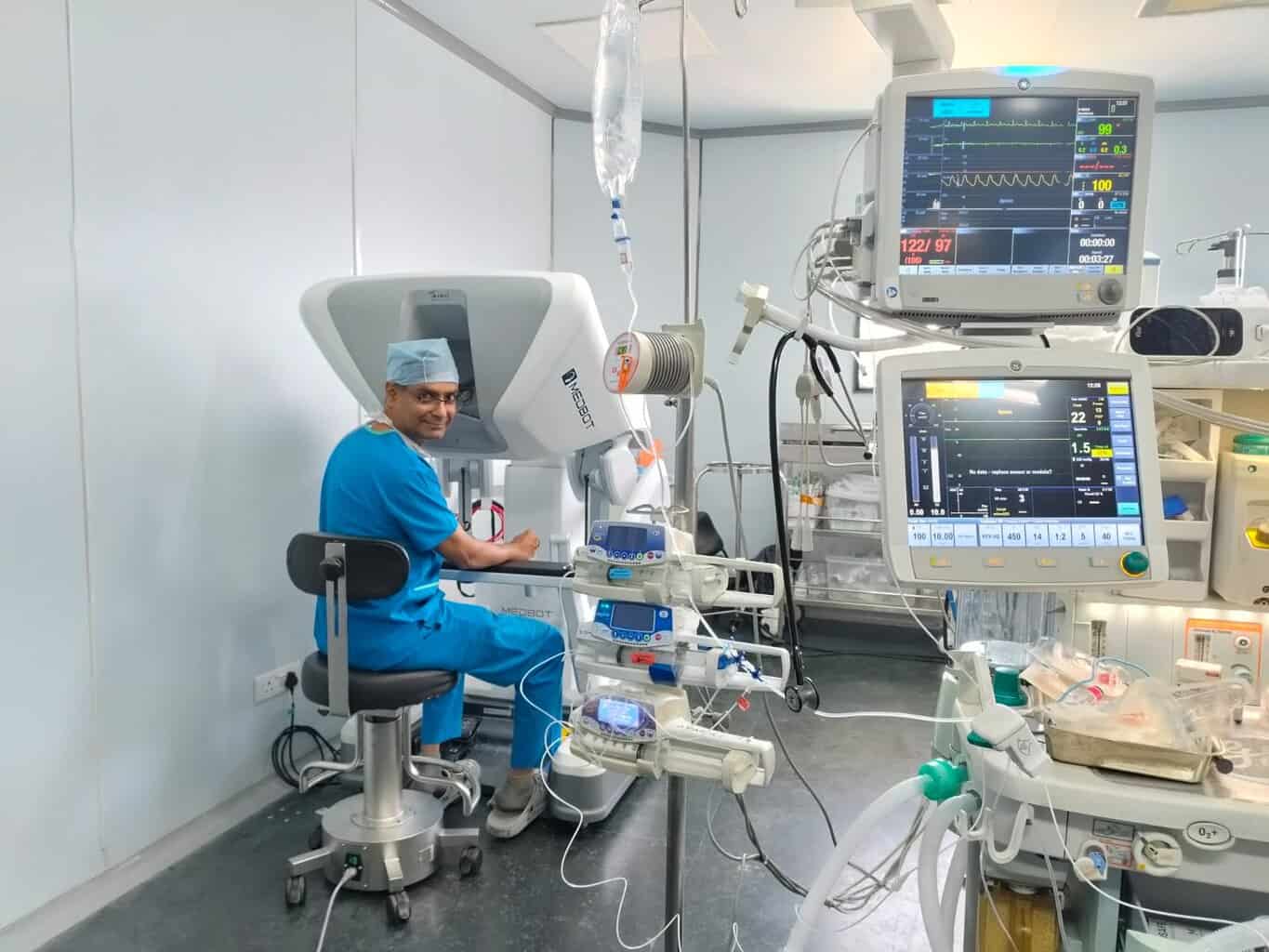
Minimally invasive cancer surgery is a way of performing surgery using small cuts instead of a large opening. Through these small cuts, a camera and specialized instruments are inserted into the body. The camera gives a magnified view of the organs and tissues, helping the surgeon operate with precision.
Depending on the cancer type and location, minimally invasive cancer surgery may include:
This approach may be used in cancers of the stomach, colon, rectum, esophagus, liver, pancreas, kidney, uterus, ovary, lung, and selected other cancers, depending on the patient’s stage and surgical plan.
The purpose is not only to reduce the size of the cut. The purpose is to perform cancer surgery safely, effectively, and with less trauma to the body where possible.


+

+

+

+

The camera provides a magnified view of the inside of the abdomen, helping the surgeon operate with precision. This approach may be used in selected cancers of the stomach, colon, rectum, uterus, ovary, kidney, adrenal gland, and other abdominal or pelvic organs.
In suitable patients, laparoscopic surgery may help reduce pain, shorten hospital stay, and support faster recovery. However, it is recommended only when complete and safe cancer removal is possible.

Robotic surgery can be useful in areas where fine precision is required, especially in deep or narrow spaces such as the pelvis, chest, or upper abdomen. It may be considered in selected cases of rectal cancer, prostate cancer, uterine cancer, esophageal cancer, stomach cancer, and other complex cancer surgeries.
The main advantage of robotic surgery is better instrument movement, three-dimensional vision, and improved control in difficult surgical areas. But robotic surgery is not required for every cancer. The decision should be based on real benefit, not only technology.

Instead of opening the chest widely, the surgeon uses small cuts and a camera to operate inside the chest cavity. This approach may be used for selected lung cancers, mediastinal tumors, thymic tumors, chest wall conditions, and some esophageal cancer procedures.
Thoracoscopic surgery may help reduce pain, breathing difficulty, and recovery time when compared with traditional open chest surgery in suitable patients. However, if the tumor is large, close to major blood vessels, or technically complex, open surgery may be safer.

In carefully selected early-stage cancers or pre-cancerous lesions, endoscopic procedures may help remove abnormal tissue without major surgery. These techniques may be used in selected cases involving the food pipe, stomach, colon, rectum, or other internal organs.
However, endoscopic treatment is suitable only for very early lesions where the cancer has not deeply invaded or spread to lymph nodes. Proper staging and biopsy review are very important before choosing this approach.

Instead of removing many lymph nodes, the surgeon identifies and removes only the first key lymph node or nodes that are most likely to receive cancer spread. These nodes are then tested in the laboratory.
This approach can reduce the need for more extensive lymph node removal in suitable patients and may lower the risk of swelling, stiffness, and long-term discomfort. It must be done carefully, because lymph node status is an important part of cancer staging and treatment planning.

For example, selected patients may benefit from breast-conserving surgery, sphincter-preserving surgery for rectal cancer, limb-sparing surgery for bone or soft tissue tumors, or organ-preserving approaches in early cancers.
The goal is to remove the cancer completely while preserving normal function as much as possible. This requires careful planning, proper imaging, and cancer-specific surgical expertise.

These may be considered in carefully chosen cases, especially for certain liver tumors, small metastatic deposits, or patients who may not be fit for major surgery. Examples include radiofrequency ablation, microwave ablation, and other liver-directed therapies.
These procedures are not replacements for surgery in every patient. They are used when they fit the overall cancer treatment plan and when they offer a safe and meaningful benefit.

Minimally invasive surgery may be considered in many cancer operations, but only after careful evaluation. The decision depends on several factors, including the cancer type, size, stage, location, spread, previous surgeries, and the patient’s overall fitness.
This approach may be used in selected cases of:
For example, a small tumor in an early stage may be suitable for minimally invasive surgery. But a large tumor involving nearby organs may require open surgery for safer and more complete removal.
I always explain why a particular approach is being recommended. If minimally invasive surgery is safe, I discuss it. If open surgery is better for cancer clearance, I explain that clearly too.
In suitable patients, minimally invasive cancer surgery may offer several advantages.
Possible benefits include:
These benefits can make a real difference, especially for patients who are worried about recovery and quality of life after surgery.
However, minimally invasive surgery also has limitations.
It may not be the best option when:
Sometimes, a surgery may begin as minimally invasive but may need to be converted to open surgery if that becomes safer during the operation. This is not a failure. It is a responsible surgical decision.
The safest and most effective approach matters more than the size of the incision.

Minimally invasive cancer surgery requires more than instruments and equipment. It requires planning, anatomical understanding, cancer-specific training, and the judgment to know when this approach is appropriate.
In cancer surgery, the surgeon must think beyond removing the visible tumor. The operation may also involve removing lymph nodes, maintaining safe margins, protecting important organs, and planning reconstruction in selected cases.
A good surgical oncologist does not choose a method just because it is available. The right surgeon chooses the approach that gives the patient the best chance of safe recovery and good cancer control.
Experience matters because every cancer behaves differently. Even two patients with the same cancer may need different surgical plans depending on stage, body structure, age, fitness, and response to previous treatment.
As a Minimally Invasive Cancer Surgeon in Bangalore, my approach is to combine advanced surgical techniques with careful clinical judgment. I will always explain the reason behind the recommendation, including when open surgery may be more appropriate.

Before surgery, I first review your diagnosis in detail. This may include biopsy reports, CT scan, MRI, PET-CT, endoscopy, colonoscopy, blood tests, cardiac evaluation, anesthesia fitness, and other relevant investigations.
The purpose of this assessment is to answer important questions:
Once the surgical plan is clear, you and your family will be guided about admission, fasting, medications, anesthesia, expected hospital stay, and recovery.
After minimally invasive cancer surgery, many patients are encouraged to sit up, walk, breathe deeply, and start gradual recovery early, depending on the type of operation. Pain control, diet progression, wound care, physiotherapy, and follow-up are explained clearly.
Hospital stay varies based on the type of cancer surgery. Some procedures may need only a short stay, while complex cancer operations may require longer monitoring.
After discharge, follow-up visits are important. We review wound healing, final biopsy reports, diet, activity, and whether further treatment such as chemotherapy or radiation is required.

Many patients ask about the Cost of Minimally Invasive Cancer Surgery in Bangalore during their first consultation. This is an important and practical question, especially when families are planning treatment, insurance, and hospital admission.
There is no single fixed cost for minimally invasive cancer surgery because every case is different.
The cost may depend on:
Robotic surgery may cost more than standard laparoscopic or open surgery because of equipment and consumable costs. However, in some patients, faster recovery and shorter hospital stay may help balance part of the overall treatment burden.
During consultation, once your reports are reviewed and the likely surgical plan is clear, the hospital team can provide a more realistic estimate. I avoid giving vague or misleading cost promises without understanding the case properly.

I currently consult at:
These centres provide access to comprehensive cancer care within a well-equipped hospital environment, supporting multidisciplinary treatment, investigations, and post-operative care when required.
Consultation timings and appointment details can be arranged through phone or WhatsApp for convenience.
